Physician associates
Physician Associates (PAs) were introduced in the UK in 2003. In the USA they are called Physician assistants where they have been present since the 1960s [1]. They are defined as “Healthcare professionals who work under the supervision of a doctor within multi-disciplinary teams” [2]. At Brunel University London, we have been running the PA programme as a 2-year, postgraduate Masters course since 2016. Students must have an undergraduate degree in a health science in order to apply to PA courses in the UK.
Since December 2024, The General Medical Council (GMC) has become the regulating body for PAs in the UK [2]. After qualifying from a University PA course, students are expected to complete national OSCE (Objective Structured Clinical Exam) and written exams before being able to practice. PAs at Brunel University London (BUL) are currently taught through Problem-based learning (PBL), Case-based learning and lecture-based learning. Our university has recently introduced a medical school with their first intake in 2022. This is a unique MBBS course with the majority of teaching delivered using Team-Based Learning. We wanted to assess TBL as a teaching method for PA students.
Team-based learning
Team-based learning is a learning strategy first developed by Larry Michaelsen in the 1970s [3]. It can be summarised into the following 3 stages:
-
1.
Preparation: Preparatory material is sent to students before the session. This can include recorded lectures, chapters in a book or guidelines. Students are required to study this before coming to the session.
-
2.
Readiness Assurance Tests: In this process, students undertake an individual test called the individual readiness assurance test (iRAT). This is then followed by the students undertaking the same test but within their team of 6–8 peers. This is called the team readiness assurance test (tRAT). At this stage, the correct answer to each question is revealed to the ‘team leader’ and students discuss further submitting their selections until they arrive at the correct answer.
-
3.
Application Exercise: Each team is then given new practical questions to solve by applying the knowledge they have gained from the first 2 stages. These questions usually consist of real-life clinical scenarios.
This process, with further steps within each stage, is summarised in Fig. 1.
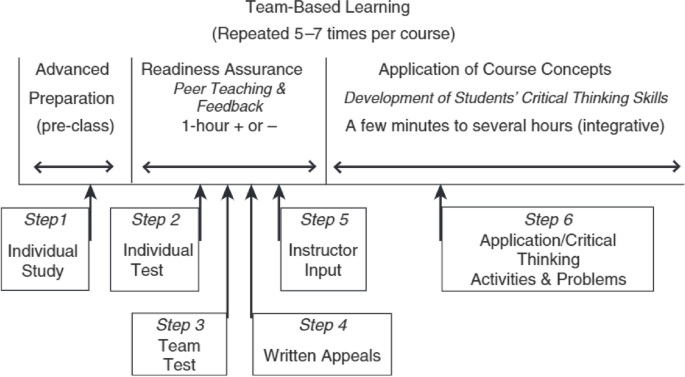
Instructional activity sequence for TBL content unit [4]
TBL and PA education
The authors did not find any specific literature outlining the type of teaching available to PA students at different universities. However, from our experience with the PA Schools Council (PASC) we know that this consists mainly of lecture-based teaching and Problem-based Learning (PBL). Our students have a PBL session once a week. The rest of their teaching is lecture-based or practical clinical skills teaching. At the largest PA course in the UK, the main teaching methods include lectures, problem-based learning (PBL), and self-directed learning [5].
A literature search identified only 4 studies that specifically explored TBL and PA students [6,7,8,9]. All these studies took place in the USA with no UK studies. One of these studies had a mixed sample of PA and nursing anaesthetic students [7]. All these articles looked at small samples of PA students ranging from 27 to 67 students in each study. Additionally, one of our authors recently published an abstract reviewing the first TBL session in a UK PA programme in a small sample of 17 PA students [10]. These studies all ranged from being purely qualitative exploring student perceptions to mixed studies that also compared exam performance between PA cohorts taught with or without TBL. The results of these studies can be divided into those looking at student performance and those exploring student perceptions.
TBL and PA student’s performance
Isbell et al. [7], Nguyen et al. [6] and Patel et al. [9] evaluated TBL for teaching gross anatomy, clinical pharmacology and Paediatric preventative medicine, respectively. Table 1 summarises these studies.
Isbell et al. [7] investigated a cohort of PA and nurse anaesthetist (NA) students. They found that the 2014 cohort who were taught using TBL performed significantly better in written and practical examinations compared to their 2013 cohort who were taught through traditional lectures and laboratory teaching only (p < 0.05).
Nguyen et al. [6] compared their 2013 PA student cohort (n = 36) who were taught by lectures only, with their 2014 PA student cohort (n = 35) who were taught by a combination of lectures and TBL. They found no significant difference between the two groups in their summative exam scores (p = 0.24). However, this study was limited as it excluded the 3rd application phase of TBL which it can be argued is essential as it resembles clinical practice [6].
Patel et al. [9] evaluated TBL in teaching a new Paediatric subject in their course entitled ‘Nutrition and Preventative Medicine across the lifespan’. They found a significant improvement in the test results of the students after TBL (p < 0.05). This simply showed that TBL improved students’ knowledge after the teaching session. There was no control group.
An additional study by Loftin and West [8] conducted a self-efficacy survey pre-intervention and post-intervention on 87 PA students who were randomised to either TBL or non-TBL learning (via online modules). Their outcome measure was ‘self-efficacy’ (confidence) and they found areas of increased confidence in the student group taught using TBL compared to the control group who learned through online modules (p < 0.05).
TBL and PA students’ perceptions
Two of the above performance studies were mixed and looked at qualitative data in addition to the performance measures. Nguyen et al. [6] and Patel et al. [9] used similar themes in their student feedback questions post-TBL teaching to evaluate student perceptions. The results are summarised in Table 2.
In general, most students had a positive perception of TBL in the context of the studies. Feedback around lack of preparation time is important and relevant to an intensive PA course. It highlights that the introduction of TBL in addition to its preparation time can be challenging. We found similar outcomes in our evaluation of a single TBL session on Stroke medicine [10].
To add to the above data, we wanted to explore student perceptions of TBL delivered over an entire module within our UK PA programme.
Geriatric medicine
Geriatric medicine or elderly care encompasses a range of chronic conditions that are covered within different specialities of our foundations of clinical medicine study block [11]. The topics that are taught each year through lectures are as follows:
-
1.
Geriatric Giants
-
2.
Delirium and the Dementias
-
3.
Stroke medicine
-
4.
Frailty
-
5.
Falls
We felt that this specialty combines teaching from multiple areas of clinical medicine. It therefore lends itself well to team-based learning with clinical application exercises. Therefore, for our 2023 cohort, we decided to deliver these topics through 4 TBL sessions and explore students’ perceptions of this teaching method.
link

